Frequently Asked Questions About Vascular Care
Scheduling & First Visit
-
We pride ourselves on prompt care—new patients are typically seen within a few business days. You don’t always need a referral; it depends on your insurance plan. If you’re unsure, contact your primary doctor or give us a call and we’ll verify your requirements.
-
Please bring a government-issued ID, your insurance card, any referral paperwork your plan requires, a list of current medications (including dosages), and any relevant medical records or imaging reports.
-
Your first appointment includes a comprehensive review of your medical history and symptoms. When needed, we can perform diagnostic imaging during the same visit to help us develop an immediate treatment plan—so there’s no waiting for answers.
Procedures & Sedation
-
Our procedures are designed to be as comfortable as possible. They’re performed under local anesthesia with mild sedation if necessary, so you stay awake but relaxed.
Most patients report little to no discomfort. Additional sedation options may be available if you’re anxious.
-
Most procedures take under an hour and are done in our office. You’ll go home the same day and typically resume light activities within 24–48 hours.
We recommend avoiding strenuous exercise for about two weeks to ensure proper healing.
-
If you receive sedation, you’ll need someone to drive you home and stay with you for 24 hours.
Insurance & Privacy
-
We accept most major insurance plans. Coverage depends on the specific procedure and whether it’s considered medically necessary.
Our billing team will obtain pre-authorizations if required and can help explain any co-payments or deductibles. Please contact your insurer for details; we’realso happy to help.
-
Your privacy is paramount. We adhere to strict confidentiality practices and will not release your medical information without your consent.
Our patient portal lets you update medical information, request appointments, and make secure payments at your convenience.
After-Care & Risks
-
Untreated vascular disease can lead to serious complications—such as blood clots, infections, ulcers and even limb loss.
After your procedure, you’ll go home with a bandage or compression wrap.
Keep the treated leg elevated, avoid heavy exertion, follow the wound-care instructions, and call us immediately if you experience unusual pain, bleeding, fever or signs of infection.
-
For clinical questions, scheduling, or follow-up concerns during business hours, please call the office where you were treated (see contact information below).
If you have an urgent issue outside business hours, call the same number, and our after-hours service will connect you with the on-call physician.
-
Absolutely. Our OBL meets strict safety and sterilization standards.
You receive hospital-level care without the inconvenience or infection risks associated with hospital stays.
We offer rapid scheduling, same-day diagnostics, minimally invasive treatments, and continuous care from board-certified vascular specialists.
Because we’re focused on below-the-waist vascular care, you benefit from a high level of expertise.
Diagnosis & Treatment
-
A vascular specialist diagnoses and treats conditions that affect blood circulation, including peripheral artery disease (PAD), venous disease, and other vascular disorders.
-
Yes. Many vascular treatments such as angioplasty, stenting, and atherectomy can be performed in specialized outpatient vascular centers, allowing patients to return home the same day.
-
Common symptoms include leg pain while walking, cramping, numbness, wounds that do not heal, and cold or discolored feet.
Conditions & Symptoms
-
We focus solely on vascular diseases below the waist. That includes:
Peripheral artery disease (PAD)
Critical limb ischemia
Varicose and spider veins
Venous insufficiency
Diabetic foot complications and non-healing wounds
Symptoms to watch for include:
Leg pain or cramping when walking
Swelling
Skin discoloration
Visible veins
Ulcers or sores
Persistent wounds.
If you notice these signs, schedule an evaluation right away.
-
Simple daily habits can make a meaningful difference in circulation and overall vascular health:
Walk at least 30 minutes a day. Regular walking improves blood flow, strengthens calf muscles and helps your veins move blood back toward your heart.
Maintain a healthy weight. Excess weight increases pressure on your blood vessels and can worsen circulation problems.
Stop smoking. Smoking damages blood vessels, accelerates plaque buildup and significantly increases the risk of peripheral artery disease and limb complications.
Eat a heart-healthy diet. Focus on lean proteins, vegetables, fruits, whole grains and healthy fats while limiting processed foods, excess sugar and saturated fats.
Avoid prolonged sitting or standing. If your job requires it, take short movement breaks every 30–60 minutes.
Elevate your legs when resting. This helps reduce swelling and supports venous return.
Manage blood pressure, cholesterol and diabetes. Keeping these conditions controlled reduces strain on your arteries and veins.
These steps not only reduce symptoms but also slow disease progression and help prevent more serious vascular complications.
-
PAD is caused by plaque buildup in the arteries that supply blood to the legs and feet.
It commonly leads to cramping or aching in the leg muscles during walking or exercise that improves with rest.
Other signs include cold feet, numbness or weakness in the legs, shiny or discolored skin, slowgrowing toenails, sores that don’t heal, and hair loss on the legs.
Early diagnosis and treatment reduce the risk of complications.
-
CLI is the most severe form of PAD, where blood flow to the legs or feet is drastically reduced.
It causes constant foot or leg pain—often even at night—and may include cold, numb or weak feet, shiny smooth skin without hair, slow healing sores or ulcers, thickened toenails, and skin discoloration or signs of gangrene.
CLI is a medical emergency; prompt treatment preserves tissue and reduces the risk of amputation.
-
Varicose veins are enlarged, bulging veins that often appear blue or purple.
They can cause heavy or tired legs, itching, aching or cramping (especially behind the knees), swelling, skin discoloration and, in severe cases, ulcers.
Spider veins are smaller red, blue or purple lines near the surface of the skin; they are usually cosmetic but can occasionally cause mild itching or burning.
Both conditions result from faulty valves in the veins but differ in size and severity.
-
Venous insufficiency occurs when the valves in the leg veins don’t work properly, so blood pools in the legs rather than returning to the heart.
Symptoms include:
Achy or heavy legs
Burning or tingling sensations
Nighttime leg cramps
Reddish-brown skin discoloration
Swelling in the lower legs and ankles
Flaking or itching skin
Heaviness or tightness in the legs
Leathery skin
Ulcers near the ankles
The presence of varicose veins
-
Diabetes can damage nerves and reduce blood flow, making the feet more susceptible to injury and infection.
Warning signs include:
Cuts, blisters, sores or calluses
Frequent bleeding
Discharge of fluid or pus
A foul smell
Pain or tenderness
Skin discoloration
Swelling
Because wounds may heal slowly, early evaluation is critical to prevent infection or tissue loss.
Our Locations
-
7402 John Smith Dr, San Antonio, TX 78229
Phone: (210) 8174848 | Fax: (210) 2576949
Hours: Monday–Friday 8 AM–5 PM; Closed Saturday & Sunday
-
8611 N Mopac Expy, Suite 250, Austin, TX 78759
Phone: (512) 221-2776 | Fax: (512) 737-8454
Hours: Monday–Friday 8 AM–5 PM; Closed Saturday & Sunday
-
1255 Ashby Street, Seguin, TX 78155
Phone: (830) 590-8049 | Fax: (806) 701-6295
Hours: Monday–Friday 8 AM–5 PM; Closed Saturday & Sunday
-
1533 5th Street, Suite A, Corpus Christi, TX 78404
Phone: (361) 266-2233 | Fax: (877) 414-0825
Hours: Monday–Friday 9 AM–4 PM; Closed Saturday & Sunday
When the arteries in your legs become narrowed or blocked, reducing blood flow. This can cause leg pain when walking, cramping, cold feet, slow-healing wounds, or changes in skin color.
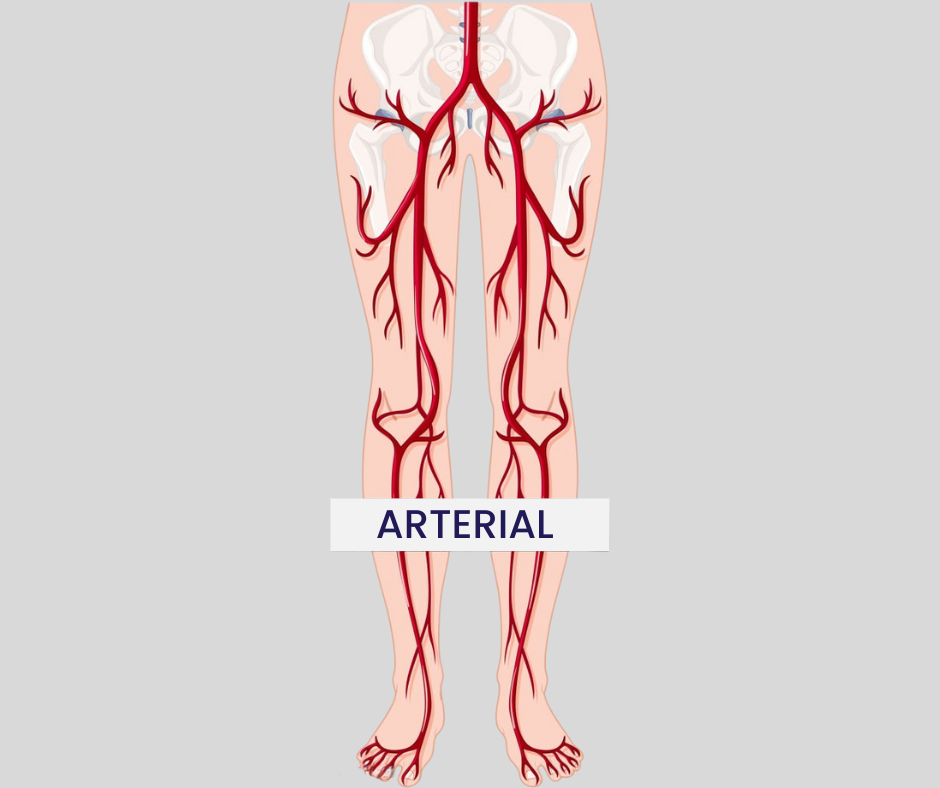
Arterial Conditions
-
When the arteries in your legs become narrowed or blocked, reducing blood flow. This can cause leg pain when walking, cramping, cold feet, slow-healing wounds, or changes in skin color.
-
A severe form of poor circulation where blood flow to the leg or foot is very limited. Symptoms can include constant pain, color changes, sores that won’t heal, or tissue damage. This condition needs urgent care.
-
Pain, cramping, or tightness in the legs that happens when walking and improves with rest. It’s often a sign of reduced blood flow in the arteries.
-
Long-term, severe circulation problems that can cause ongoing pain, wounds, or infections in the foot or leg. Without treatment, it can put the limb at risk.
-
Narrowing of the arteries in the neck that supply blood to the brain. This can increase the risk of stroke and may cause symptoms like dizziness or vision changes—or no symptoms at all.
-
Narrowing of the arteries that supply blood to the kidneys. This can affect blood pressure control and kidney function.
-
A sudden loss of blood flow to a leg or arm. Symptoms may include sudden pain, coldness, numbness, or color changes. This is a medical emergency.
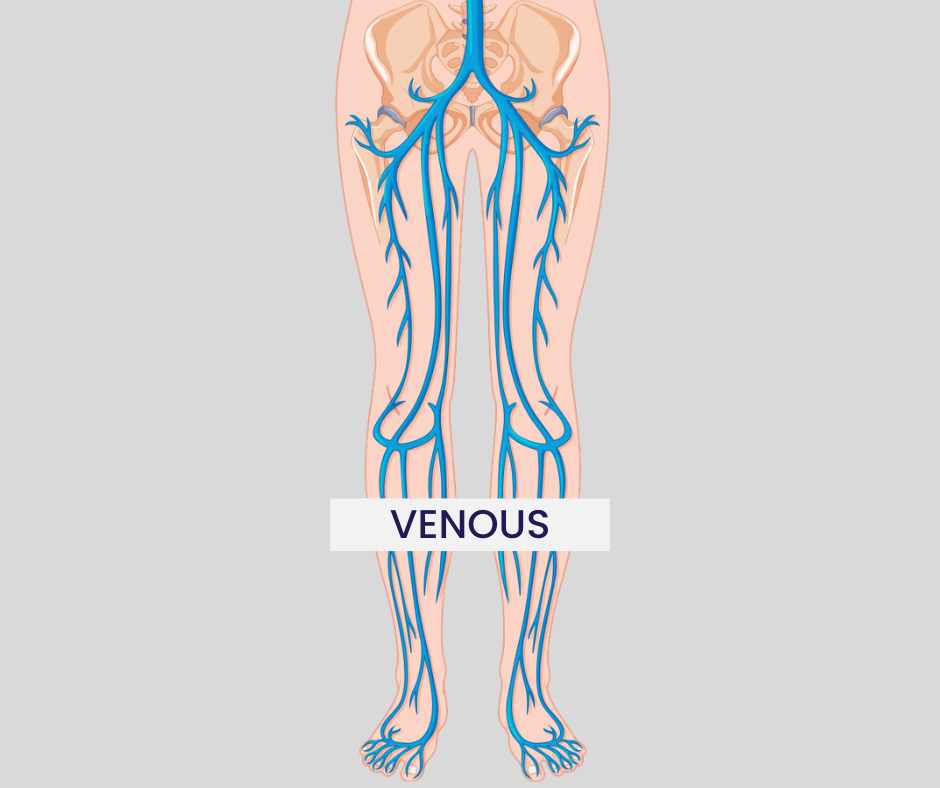
Venous conditions affect the veins that carry blood back to the heart. When blood doesn’t flow properly, it can cause leg swelling, aching, heaviness, skin changes, or varicose veins.
Venous Conditions
-
When the veins in the legs don’t move blood back to the heart properly, causing blood to pool. This can lead to leg swelling, aching, heaviness, skin discoloration, or fatigue in the legs.
-
Enlarged, twisted veins that are visible under the skin, often in the legs. They can cause aching, heaviness, throbbing, or swelling and may worsen with long periods of standing or sitting.
-
A condition where vein valves don’t close properly, allowing blood to flow backward and pool in the legs. This can cause swelling, pain, skin changes, or varicose veins.
-
Open sores on the lower leg or ankle caused by poor blood flow in the veins. These wounds can be slow to heal and may come back without proper treatment.
-
A blood clot that forms in a deep vein, usually in the leg. Symptoms may include swelling, pain, warmth, or redness. This condition requires prompt medical attention.
-
A blood clot in a vein close to the surface of the skin. It can cause redness, tenderness, and swelling along the vein and is usually less serious than a deep clot but still needs evaluation.